ZURICH — Doctors tracking vision in children with myelin oligodendrocyte glycoprotein antibody-associated disease, or MOGAD, found optical coherence tomography scans reveal lasting retinal changes better than other tests. The rare autoimmune condition often strikes the optic nerves, causing inflammation, but kids usually regain good sight. Structural damage lingers.
Researchers in Switzerland recruited 12 patients averaging 10.9 years old, all confirmed positive for MOGAD antibodies. They matched each with a healthy control child around 11.5 years old. Everyone got a full battery of eye exams: pattern-reversal visual evoked potentials at 15- and 60-minute check sizes, spectral-domain OCT for retinal layers, high- and low-contrast distance visual acuity, near visual acuity, and color vision checks.
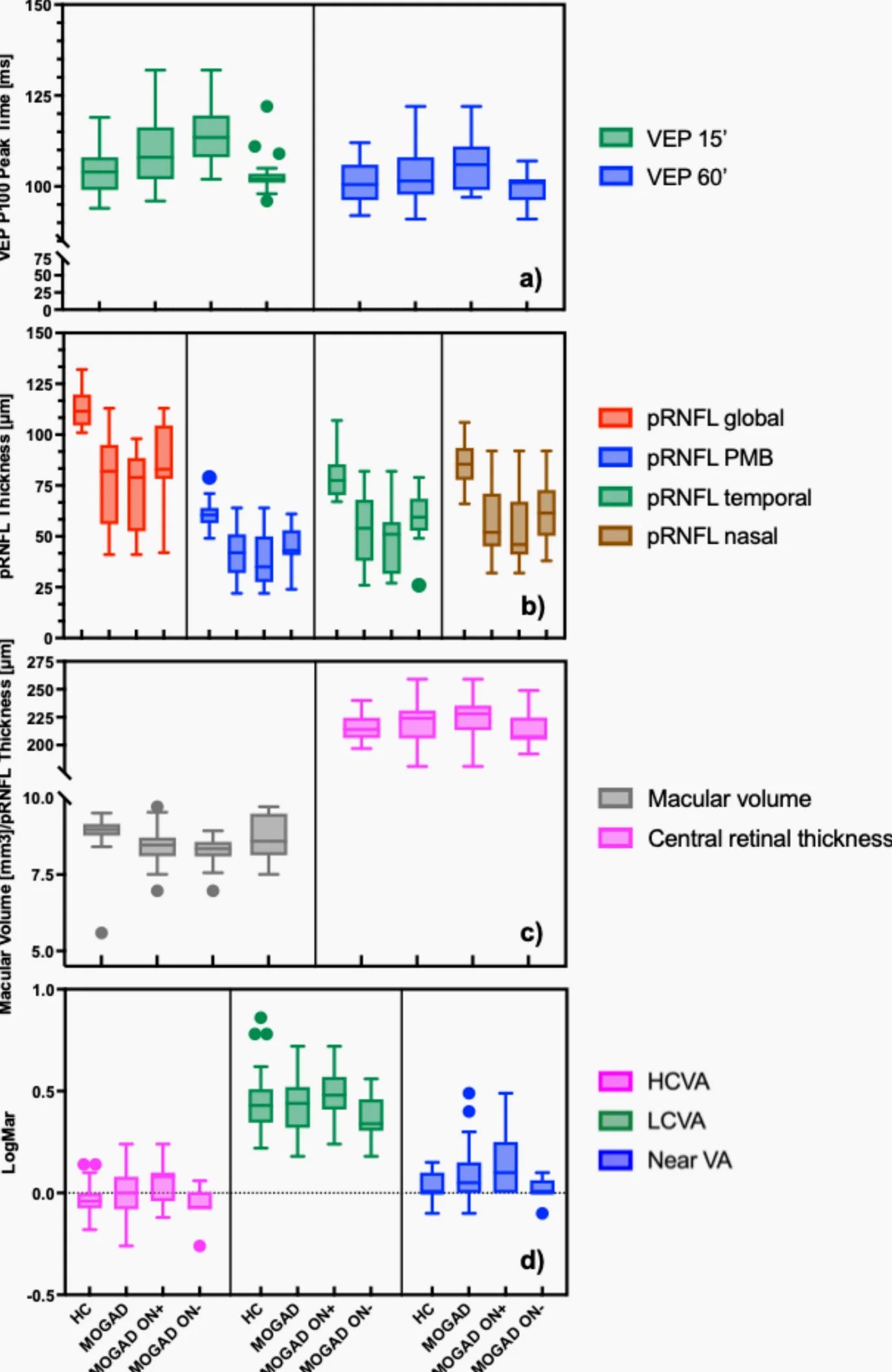
VEP measured P100 peak times, key signals from the visual pathway. OCT gauged peripapillary retinal nerve fiber layer thickness in global, temporal, nasal, and papillomacular bundle sectors, plus macular volume and central retinal thickness. The team crunched discriminative power with receiver operating characteristic analysis.
Results showed VEP P100 times mostly matched between patients and controls. Retinal nerve fiber layer readings dipped lower in MOGAD kids across the board. ROC curves gave excellent to outstanding separation for global, papillomacular bundle, temporal, and nasal sectors—overall, and split by eyes with or without past optic neuritis.
VEPs fared worse, with fair or poor overall discrimination. The smaller 15-minute checks bucked that trend, sharply distinguishing inflamed eyes from healthy ones. Low-contrast acuity and color tests didn’t shine in picking out disease eyes.
“OCT-derived pRNFL thickness differentiated MOGAD from controls with high accuracy, including in eyes without prior ON,” the study states. VEPs offered limited help, cementing OCT as the go-to for subclinical structural hits.
MOGAD hits the central nervous system, with optic neuritis the frequent opener in kids. Past work notes good functional bounce-back, but scans like OCT catch persistent thinning. This study pushes OCT as a biomarker, even sans symptoms.
Patients hailed from across Switzerland, ensuring a real-world mix. No major vision loss marked the group, mirroring MOGAD’s kinder course versus multiple sclerosis or aquaporin-4 neuromyelitis optica. Still, early detection matters for monitoring and trials.
Experts see promise. Thinner nerve fibers signal axonal loss, a stealth threat. OCT’s non-invasive snap—quick, repeatable—fits pediatric clinics. Future work could track changes over time or test treatments.
The findings appear in Documenta Ophthalmologica. Lead authors from University Hospital Zurich’s ophthalmology team ran the show, with support from Swiss National Science Foundation grants. Twelve per group keeps stats solid for rarities like MOGAD, hitting about 1 in 100,000 kids yearly.
Clinicians now eye OCT for routine MOGAD checks. It spots trouble before vision falters, guiding care in this demyelinating puzzle.








Comments
No comments yet
Be the first to share your thoughts